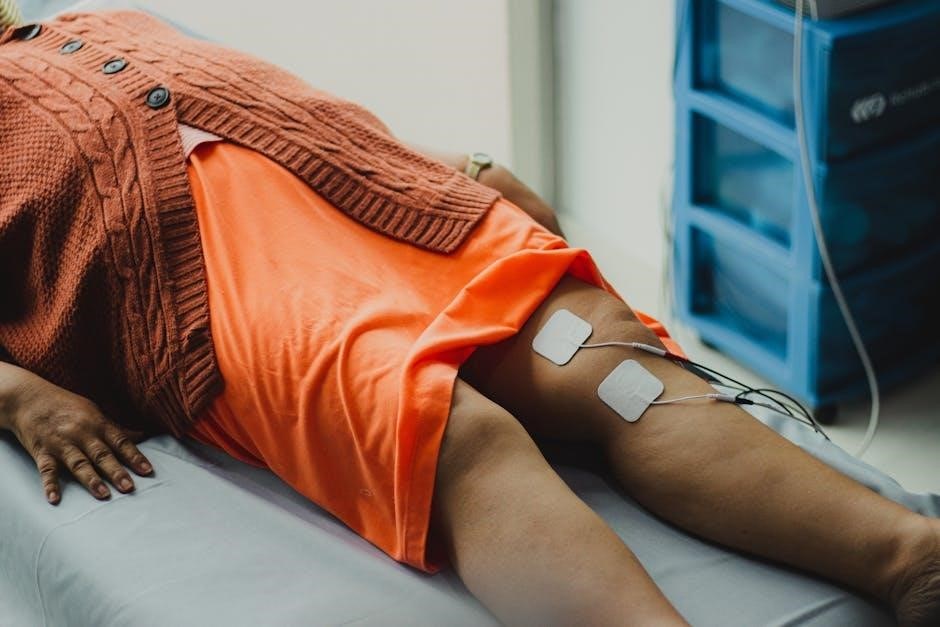
Understanding Baker Cyst Treatment
Effective treatment strategies encompass conservative approaches like NSAIDs and analgesics, alongside interventions such as aspiration, corticosteroid injections, and surgical options when necessary.
What is a Baker Cyst?
A Baker cyst, also known as a popliteal cyst, is a fluid-filled sac that develops behind the knee. This condition arises due to an underlying issue within the knee joint, causing excess synovial fluid production. The cyst typically forms a noticeable bulge and can cause stiffness and discomfort. It’s not the primary problem, but rather a symptom of another knee condition like arthritis or a cartilage tear.
The cyst develops when synovial fluid, which lubricates the knee joint, bulges out through a weak area in the joint capsule. This creates a pocket of fluid behind the knee. While often painless, a Baker cyst can become problematic if it grows large enough to cause pain, limit range of motion, or rupture. Understanding the root cause is crucial for effective treatment.
Causes and Contributing Factors
Several factors contribute to Baker cyst development, primarily underlying knee joint issues. Osteoarthritis is a significant cause, leading to inflammation and increased synovial fluid. Meniscal tears, cartilage damage, and ligament injuries also disrupt normal knee function, prompting fluid buildup. The presence of a one-way valve within the joint capsule allows fluid to leak into the cyst but prevents it from returning.
Rheumatoid arthritis and other inflammatory conditions can exacerbate the problem. Trauma to the knee, even without a direct injury to the cyst itself, can trigger fluid accumulation. Age and pre-existing knee conditions increase susceptibility. Addressing these underlying pathologies is essential for long-term relief and preventing cyst recurrence, often requiring arthroscopic intervention.
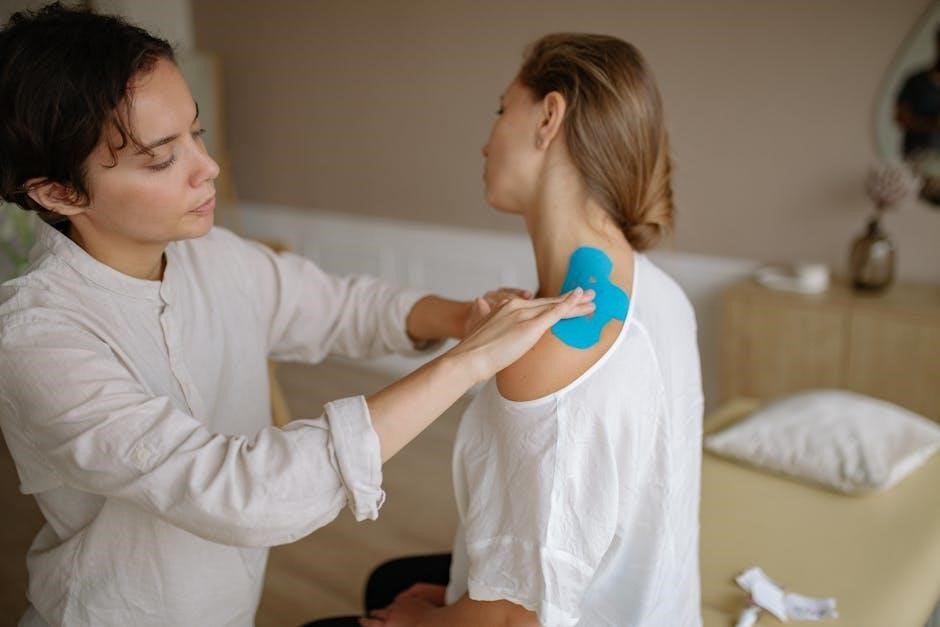
Non-Surgical Treatment Options
Initial management focuses on conservative measures: NSAIDs for inflammation, analgesics for pain, and potentially aspiration alongside corticosteroid injections for symptom relief.
Conservative Management
Conservative management represents the first line of defense in treating Baker cysts, aiming to alleviate symptoms without resorting to more invasive procedures. This approach typically involves a combination of rest, ice, compression, and elevation – often referred to as the RICE protocol – to reduce swelling and discomfort. Activity modification is crucial; avoiding activities that aggravate the knee is paramount.
Furthermore, gentle range-of-motion exercises can help maintain joint flexibility and prevent stiffness. While conservative measures may not eliminate the cyst itself, they can effectively manage symptoms, particularly in milder cases. It’s a foundational step before considering other treatment avenues, offering a non-pharmacological approach to initial symptom control and potential long-term management.
NSAIDs (Nonsteroidal Anti-inflammatory Drugs)
Nonsteroidal anti-inflammatory drugs (NSAIDs) play a significant role in managing Baker cyst symptoms by reducing pain and inflammation within the knee joint. These medications work by inhibiting the production of prostaglandins, substances that contribute to both pain and swelling. Common over-the-counter NSAIDs include ibuprofen and naproxen, while stronger prescriptions are also available.
However, prolonged NSAID use can carry potential side effects, such as gastrointestinal issues and cardiovascular risks, necessitating careful consideration and physician guidance. They address the underlying inflammation contributing to cyst development and discomfort, offering symptomatic relief. NSAIDs are often used in conjunction with other conservative treatments, forming a core component of initial pharmacological management.
Pain Management with Analgesics
Analgesics, or pain relievers, offer symptomatic relief for Baker cyst discomfort, though they don’t address the underlying cause. These medications range from over-the-counter options like acetaminophen to stronger, prescription-only opioids in severe cases. Acetaminophen primarily reduces pain, while opioids provide more potent pain relief but carry a higher risk of side effects and dependence.
Analgesics are frequently used alongside NSAIDs and other conservative treatments to manage pain levels and improve patient comfort. Their role is crucial in allowing patients to participate in physical therapy and other rehabilitative exercises. It’s important to note that analgesics are best utilized as part of a comprehensive treatment plan, not as a standalone solution, to effectively manage Baker cyst symptoms.
Aspiration of Cyst Fluid
Aspiration involves using a needle and syringe to remove fluid from the Baker cyst, providing temporary relief from pressure and discomfort. This procedure is often performed in a doctor’s office and can be guided by ultrasound or fluoroscopy for increased accuracy. While aspiration can quickly reduce swelling and pain, it doesn’t address the underlying cause of the cyst formation.
Often, aspiration is combined with corticosteroid injection to reduce inflammation and prolong the pain relief. However, recurrence is common after aspiration alone, highlighting the need to address the root issue, such as underlying joint pathology. It’s a valuable diagnostic tool, allowing analysis of the fluid to rule out other conditions, and a useful palliative measure.
Corticosteroid Injections
Corticosteroid injections directly into the Baker cyst offer a more sustained anti-inflammatory effect than aspiration alone. These injections reduce swelling, pain, and inflammation within the cyst, providing significant, albeit temporary, symptom relief. Often administered alongside aspiration, the corticosteroid helps prevent rapid fluid re-accumulation and addresses the inflammatory component contributing to the cyst’s size and discomfort.
However, repeated corticosteroid injections are not recommended due to potential long-term side effects on the surrounding tissues. While effective for managing symptoms, they don’t resolve the underlying cause of the cyst. Combining injections with a comprehensive treatment plan addressing joint pathology is crucial for lasting improvement and preventing recurrence, as highlighted in current literature.
Surgical Interventions
Surgical options, including open cystectomy and arthroscopic approaches, address underlying joint issues and the one-way valve mechanism contributing to cyst formation.
Open Posterior Cystectomy
Open posterior cystectomy involves a surgical incision at the back of the knee to directly remove the Baker cyst. This approach is often considered for recalcitrant cases, meaning those that haven’t responded to more conservative treatments like aspiration or injections. The procedure aims to excise the cyst completely, addressing the symptomatic bulge and relieving pressure.
However, it’s crucial to understand that simply removing the cyst doesn’t always resolve the underlying issue. Surgeons often focus on clarifying the features of the one-way valve within the joint capsule, which allows fluid to leak into the cyst. Addressing this valve mechanism, alongside excising the cyst, is vital for long-term success. This surgical intervention is frequently used in conjunction with addressing any underlying intra-articular pathologies contributing to the effusion.
Arthroscopic Surgery for Underlying Pathology
Arthroscopic surgery plays a key role in treating Baker cysts by addressing the root cause – often, underlying joint pathology within the knee. This minimally invasive procedure utilizes a small camera and instruments inserted through tiny incisions. Surgeons can identify and repair issues like meniscal tears, cartilage damage, or ligament injuries that contribute to joint effusion and, consequently, cyst formation.
Clarifying the features of the one-way valve mechanism within the joint capsule is also crucial during arthroscopy. Correcting intra-articular pathologies reduces fluid production, diminishing the pressure that fuels the cyst. This approach, sometimes combined with cyst excision, offers a more targeted and potentially durable solution than solely focusing on the cyst itself, especially in recalcitrant cases requiring supine arthroscopy.
Addressing the One-Way Valve Mechanism
Understanding and addressing the “one-way valve” within the joint capsule is paramount for effective, long-term Baker cyst treatment. This mechanism allows synovial fluid to leak into the cyst but prevents it from flowing back into the joint. Clarifying the features of this valve improves comprehension of cyst causation and justifies targeted interventions.
Surgical intervention, particularly arthroscopic surgery, can directly address this valve. By correcting intra-articular pathologies and excising the posterior cyst, the valve mechanism can be eliminated, preventing further fluid accumulation. This approach moves beyond symptomatic relief, aiming to resolve the underlying cause and reduce recurrence rates, offering a more durable solution for patients experiencing persistent issues.
Advanced Treatment Approaches
Ultrasound and fluoroscopic guidance enhance aspiration and injection accuracy, utilizing Depomedrone and Bupivacaine for durable pain reduction in many patients experiencing Baker cysts.
Ultrasound-Guided Aspiration & Injection
Ultrasound guidance provides real-time visualization during aspiration of the Baker cyst fluid, ensuring precise needle placement and maximizing fluid removal. This technique is particularly valuable for cysts that are difficult to palpate or located in complex anatomical areas. Following aspiration, a therapeutic injection, often a combination of Depomedrone (a corticosteroid) and Bupivacaine (a local anesthetic), is administered directly into the cyst cavity.
Depomedrone helps to reduce inflammation within the cyst and surrounding tissues, while Bupivacaine provides immediate pain relief. The combination aims for a durable reduction in symptoms; This approach is often favored for symptomatic Baker cysts, offering a minimally invasive alternative to surgical intervention. Studies suggest a significant proportion of patients experience sustained pain relief with this method, making it a valuable component of advanced treatment protocols.
Fluoroscopic-Guided Aspiration & Injection
Fluoroscopy utilizes real-time X-ray imaging to guide the aspiration needle into the Baker cyst, offering enhanced accuracy, especially in challenging cases or when ultrasound visualization is suboptimal. Similar to ultrasound-guided techniques, this begins with aspiration of the accumulated cyst fluid, relieving pressure and discomfort. Subsequently, a therapeutic injection is delivered directly into the cyst cavity.
The typical injection comprises Depomedrone, a potent corticosteroid to address inflammation, and Bupivacaine, a local anesthetic for immediate pain management. This combined approach aims to provide both short-term relief and longer-lasting reduction in symptoms. Fluoroscopic guidance ensures precise delivery of the medication, maximizing its therapeutic effect and minimizing the risk of complications. This method represents a valuable option within advanced treatment strategies for symptomatic Baker cysts.
Depomedrone and Bupivacaine Injections
Combining Depomedrone, a long-acting corticosteroid, with Bupivacaine, a potent local anesthetic, offers a synergistic approach to Baker cyst treatment. Depomedrone effectively reduces inflammation within the cyst and surrounding tissues, addressing the underlying cause of discomfort. Simultaneously, Bupivacaine provides immediate and substantial pain relief upon injection.
This therapeutic injection is often administered following aspiration of the cyst fluid, maximizing its impact. The corticosteroid’s prolonged action aims for durable symptom reduction, while the anesthetic offers instant comfort. Studies demonstrate that this combination, guided by either ultrasound or fluoroscopy, leads to significant pain reduction in a majority of patients, presenting a less invasive alternative to surgical interventions for symptomatic Baker cysts.
Recurrent Baker Cysts
Recurrence often stems from untreated underlying joint issues or a persistent one-way valve mechanism, necessitating further evaluation and targeted treatment strategies.
Reasons for Recurrence
Baker cyst recurrence is a frustrating issue for many patients, often stemming from factors beyond simple cyst removal. A key contributor is the failure to address the underlying joint pathology – conditions like osteoarthritis or meniscal tears – that initially caused the effusion leading to cyst formation. If these root causes remain uncorrected, fluid will continue to accumulate, potentially reforming the cyst.

Furthermore, the “one-way valve” mechanism within the joint capsule plays a crucial role. This valve allows synovial fluid to leak into the cyst but hinders its return. Even after cyst excision, if this valve remains intact, fluid can re-accumulate. Therefore, identifying and addressing this valve, often through arthroscopic surgery, is vital for long-term success. Simply draining the cyst provides only temporary relief without tackling these fundamental issues.
Treatment Strategies for Recurrent Cases
When a Baker cyst returns after initial treatment, a more comprehensive approach is essential. Initial steps often involve ultrasound or fluoroscopic-guided aspiration coupled with therapeutic injection of Depomedrone and Bupivacaine, aiming for durable pain reduction. However, this is frequently a temporary solution.
Crucially, recurrent cases necessitate a thorough re-evaluation of the underlying joint pathology. Arthroscopic surgery to address issues like meniscal tears or cartilage damage becomes paramount. Simultaneously, attention must be given to the “one-way valve” mechanism; surgical correction or excision can prevent re-accumulation. Open posterior cystectomy may be considered for recalcitrant knees, alongside addressing the valve. A personalized plan, focusing on both symptom management and root cause resolution, is key to lasting relief.
Diagnosis and Assessment
Diagnosis is typically clinical, but imaging techniques like MRI and ultrasound are valuable for confirmation and to rule out other knee pathologies.
Clinical Diagnosis
A clinical diagnosis of a Baker cyst often relies on a thorough physical examination, focusing on the patient’s history and specific symptoms. Palpation behind the knee frequently reveals a noticeable, fluid-filled mass, which may be more prominent with knee flexion. Patients commonly report discomfort or a feeling of tightness in the popliteal fossa.
However, it’s crucial to differentiate a Baker cyst from other conditions presenting similar symptoms, such as deep vein thrombosis or a soft tissue tumor. A detailed assessment of the patient’s knee joint is essential, evaluating for underlying arthritis or meniscal tears, as these are frequently associated with cyst development. The physician will inquire about any prior knee injuries or surgeries, and assess the range of motion and stability of the knee.
Imaging Techniques (MRI, Ultrasound)
While a clinical diagnosis is often sufficient, imaging techniques play a vital role in confirming the presence of a Baker cyst and evaluating underlying knee pathology. Ultrasound is a readily available and cost-effective modality, effectively visualizing the cyst as a fluid-filled sac behind the knee. It can also help differentiate the cyst from other potential causes of popliteal pain.
Magnetic Resonance Imaging (MRI) provides a more detailed assessment, revealing the cyst’s size, location, and relationship to surrounding structures. Crucially, MRI can identify any associated intra-articular abnormalities, such as meniscal tears or cartilage damage, which may be contributing to the cyst formation. This information is essential for guiding appropriate treatment strategies and addressing the root cause of the problem.
Post-Treatment Care & Rehabilitation
Following treatment, physical therapy and activity modification are crucial for restoring knee function, reducing pain, and preventing Baker cyst recurrence effectively.
Physical Therapy Exercises
A comprehensive physical therapy program is essential post-treatment, focusing on strengthening the muscles surrounding the knee joint to enhance stability and reduce stress. Initial exercises often involve gentle range-of-motion activities, like heel slides and quad sets, to restore flexibility without exacerbating pain.
Progressive strengthening exercises, including hamstring curls, calf raises, and short arc quads, gradually build muscle strength. Proprioceptive exercises, such as single-leg stance and balance board work, improve joint awareness and coordination.
Furthermore, therapists may incorporate stretching exercises to improve flexibility in the hamstrings, quadriceps, and calf muscles. A tailored program, guided by a physical therapist, ensures appropriate progression and minimizes the risk of re-injury, ultimately promoting long-term knee health and function.
Activity Modification
Following Baker cyst treatment, carefully modifying activities is crucial for optimal recovery and preventing recurrence. Initially, avoiding activities that aggravate the knee – such as deep squatting, prolonged standing, and high-impact exercises – is paramount. Gradual resumption of activities is key, guided by pain levels and functional improvements.
Individuals should consider low-impact alternatives like swimming, cycling, or walking on level surfaces. Proper footwear with good support can also minimize stress on the knee joint.
It’s important to listen to the body and avoid pushing through pain. A phased return to normal activities, under the guidance of a healthcare professional, ensures a safe and sustainable recovery, minimizing the risk of cyst reformation and promoting long-term joint health.